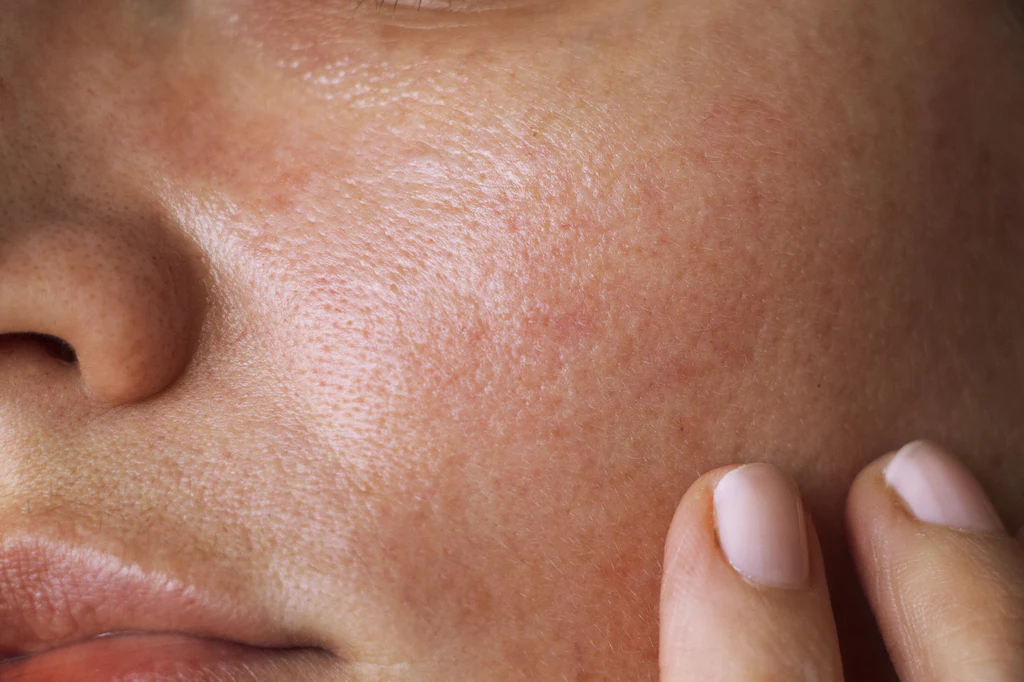
Steroid Dermatitis
Topical steroid withdrawal, or red skin syndrome, is also called
steroid dermatitis. The condition comes about after applying topical
corticosteroids on the skin for two weeks or longer and then
discontinued suddenly, bringing about withdrawal. Common withdrawal
symptoms for the condition include redness, itchiness, scabs, hot
skin, hives, fatigue, and eye problems. People with atopic
dermatitis (eczema) are most at risk. The most common treatment is
to decrease the use of the steroid cream gradually and to apply
ointments such as Vaseline to decrease symptoms.
Clara gives us her story as a person living with steroid dermatitis,
how it started, and how the experience has been so far. She shares
the stigma, depression, and anxiety associated with red-burning skin
syndrome.
Her Experience with Steroid Dermatitis
Clara's condition began in late 2020 during the height of COVID-19.
When she was prescribed a steroid cream to deal with her eczema
flare-ups around her neck and face, "I went in, and the doctor
prescribed a corticosteroid cream, Clozole B, to be applied twice a
day, in the morning and before going to bed in affected areas…"
Her eczema flare-ups had gone down, and her skin returned to normal
until about a month later when they returned, and she started
applying the cream again. She used it for two months consecutively,
saying, "I was desperate to have them [the eczema flare-ups] gone… I
was working overtime for an editorial shoot for a magazine they had
featured me on campus, so I applied the steroid, hoping for the
results I had recorded earlier."
When she stopped using her steroids, she experienced withdrawal
symptoms like never before, experiencing the severity of steroid
addiction syndrome. Clara's withdrawal, she explains, included
itchiness and redness, especially around the neck and face areas.
Clara recalls that the itching would sometimes be everywhere
simultaneously, even in areas she hadn't applied the steroid to, and
would be persistent. Her face had scabs and was always puffy and
itchy. Her skin also became severely dry, triggering the return of
her eczema.
"It was a very dark period of my life socially," she said. "People
would stare, and some asked me questions about my face. My skin
looked horrendous, and I was afraid to go in public, let alone do my
photo shoots."
She experienced anxiety, particularly in public on campus and
walking in the streets, and had severe depression afterward.
Clara feared that "the condition would remain forever, and I would
always have these nasty withdrawal symptoms."
The condition has no cure, and the recovery period depends on the
duration of use, with some having to live with withdrawal for years.
People who have applied the corticosteroids for more prolonged
periods tend to experience more severe and lasting symptoms, as the
condition may relapse years after the skin has returned to its
normal state.
Her Recovery
However, she noted some things she could do to help relieve her
pain, such as "Doing cold compresses with ice on my face has helped
with the symptoms of burning and stinging, and fortunately, my skin
is almost fully restored."
Clara, speaking from experience, advises to "Use steroid creams for
less than two weeks as per the doctor's prescription. No more. Also,
consult your dermatologist as soon as the flare-ups come back for
advice on what to do."
Joining online support groups with others recovering from red skin
syndrome is also highly recommended. It helps in the withdrawal
journey because you see and hear from others going through the same
problem and know you are not alone. There are also many success
stories to inspire and motivate others on the same journey.
Sources
https://www.ncbi.nlm.nih.gov/books/NBK424899/ https://eczema.org/information-and-advice/treatments-for-eczema/topical-corticosteroids/ https://www.webmd.com/skin-problems-and-treatments/psoriasis/topical-steroid-cream-withdrawal